Antihistamine Interaction Risk Checker
Select Your Antihistamine
Select Other Medications
Risk Assessment
Select your medications to see your risk level
Important Safety Information
Combining antihistamines with other sedating drugs can be dangerous-sometimes life-threatening. Many people don’t realize that the allergy pill they take for hay fever or the sleep aid they use on weekends can turn into a hidden risk when mixed with painkillers, anxiety meds, or even alcohol. This isn’t theoretical. Every year, over 300,000 emergency room visits in the U.S. are linked to these kinds of drug clashes, and antihistamines are involved in nearly 15% of them.
Not All Antihistamines Are the Same
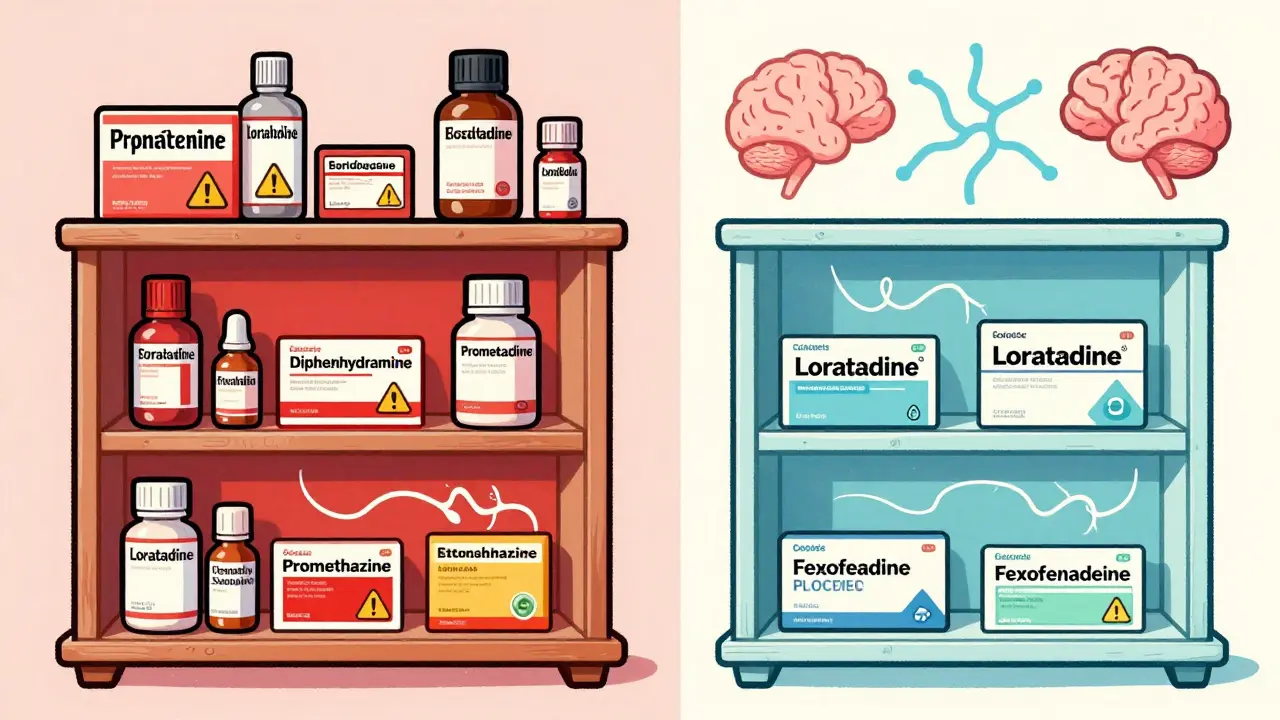
You might think all antihistamines work the same way, but that’s not true. There are two main types: first-generation and second-generation. The difference isn’t just marketing-it’s about safety.
First-generation antihistamines like diphenhydramine (Benadryl), hydroxyzine (Vistaril), and promethazine (Phenergan) are old-school drugs. They were developed in the 1940s and designed to cross the blood-brain barrier. That’s why they make you sleepy. But that same ability to enter your brain is what makes them risky when combined with other CNS depressants. They don’t just block histamine-they also mess with acetylcholine, a brain chemical critical for memory, alertness, and muscle control. This is called anticholinergic activity. Diphenhydramine scores a 3 out of 3 on the Anticholinergic Cognitive Burden (ACB) scale-the highest possible rating.
Second-generation antihistamines like loratadine (Claritin), cetirizine (Zyrtec), and fexofenadine (Allegra) were made to avoid this. They’re engineered to stay out of the brain. Thanks to special transporters in the blood-brain barrier, they can’t get in easily. That’s why they’re called "non-drowsy." Studies show 97% of users report no drowsiness with loratadine, compared to 68% who feel sleepy with diphenhydramine. Their ACB scores are 0 or 1, meaning far less risk.
What Happens When You Mix Them?
When you take a first-generation antihistamine with another sedating drug, the effects don’t just add up-they multiply. This is called synergistic CNS depression. It means your brain slows down more than either drug alone would cause.
Take benzodiazepines, like lorazepam (Ativan) or alprazolam (Xanax). A 2013 study found that diphenhydramine increased the sedative effects of lorazepam by 37% in objective tests and 42% in how people felt. That’s not a small bump-it’s a major safety concern. People reported extreme drowsiness, confusion, and trouble walking. In contrast, second-generation antihistamines like bilastine showed no such effect in the same study.
Now consider opioids. Alone, opioids cause respiratory depression in about 1.5% of users. But when paired with a first-generation antihistamine, that number jumps to 8.7%. That’s nearly six times higher. The CDC reported cases where people stopped breathing after combining codeine or oxycodone with Benadryl. One Reddit user described nearly dying after taking 50mg of diphenhydramine with 1mg of Xanax-breathing slowed so much they had to be rushed to the hospital.
Even alcohol is dangerous. One standard drink with 25mg of diphenhydramine has led to blackouts and hospital visits. WebMD data shows 41% of people who took diphenhydramine with opioids reported severe dizziness requiring medical care. Only 8% of those on opioids alone had the same issue.
Who’s at Highest Risk?
It’s not just about what you take-it’s who you are. Older adults are especially vulnerable. As we age, our liver and kidneys clear drugs more slowly. Elderly patients clear first-generation antihistamines 50-70% slower than younger people. That means even a normal dose builds up in their system, increasing the chance of falls, confusion, or delirium.
The American Geriatrics Society has been warning about this for years. Their Beers Criteria-a trusted guide for safe prescribing in older adults-lists first-generation antihistamines as "potentially inappropriate." Why? Because they’re linked to a 54% higher risk of dementia with long-term use. A 2021 JAMA Internal Medicine study found that combining diphenhydramine with other anticholinergic drugs like oxybutynin (used for overactive bladder) spiked delirium risk in seniors.
Even younger people aren’t safe if they’re on multiple meds. The average Medicare patient takes 7.8 prescription drugs. Add over-the-counter antihistamines on top of that, and you’re stacking up anticholinergic burden. One study found 58% of primary care doctors failed to spot dangerous combinations during mock patient exams. That’s not just a gap in knowledge-it’s a public health blind spot.
What Should You Do?
If you’re taking a first-generation antihistamine, ask yourself: Why? Are you using it for allergies, sleep, or motion sickness? If it’s for allergies, switch. There’s no reason to risk brain fog, falls, or worse when loratadine or fexofenadine work just as well without the danger.
Here’s a simple checklist:
- If you’re over 65, avoid diphenhydramine, hydroxyzine, and promethazine entirely.
- If you’re on opioids, benzodiazepines, sleep aids, or muscle relaxants, don’t take Benadryl or similar meds.
- Check your pill bottles. If it says "diphenhydramine," "hydroxyzine," or "promethazine," talk to your doctor or pharmacist.
- Don’t assume "non-drowsy" means safe. Cetirizine (Zyrtec) still has an ACB score of 1-so it can interact with strong sedatives.
- Use the FDA’s MedWatch system to report any bad reactions. In 2022 alone, over 2,800 adverse events were logged from antihistamine interactions.
Many pharmacies now have free tools like the Institute for Safe Medication Practices’ Antihistamine Interaction Checker. Use them. It takes two minutes. It could save your life-or someone else’s.

What’s Changing Now?
The tide is turning. Since 2018, sales of first-generation antihistamines have dropped 12.7% a year. Meanwhile, second-generation drugs now make up 83% of the U.S. OTC antihistamine market. The FDA updated labels in 2021 to include bold warnings: "WARNING: May cause severe drowsiness when combined with alcohol, opioids, or sleep medications." In January 2024, the American Geriatrics Society added hydroxyzine to its high-risk list for dementia patients. Newer antihistamines like bilastine are showing no interaction with benzodiazepines even at high doses. And research in 2024 found that people with certain genetic variants (CYP2D6 poor metabolizers) process diphenhydramine 3.2 times slower-making them far more vulnerable.
Health systems like Kaiser Permanente have cut antihistamine-related ER visits by 34% using automated drug alerts. That’s proof that awareness works. The future is clear: first-generation antihistamines will stick around for motion sickness or end-of-life care, but they’re no longer first-line for allergies. The data doesn’t lie.
Final Thought
You don’t need to suffer through allergy season to protect yourself. You don’t need to choose between relief and safety. The better option exists. It’s safer, just as effective, and doesn’t come with a hidden clock ticking in your brain. Switching isn’t a hassle-it’s a smart health move. And if you’re caring for an older loved one, this might be the most important conversation you have this year.






Write a comment
Your email address will be restricted to us